Review of Literature
The study of the management of fractured mandible is a step by step progress made over the centuries to reach today’s standards of implantation of alloplastic materials in this direction.
The 1st therepautic guidelines for mandibular fracture were laid down by Hippocrates (460 – 375 BC). Who advocated the use of Gold wire and linen thread to splint loose teeth and strips of leather, for support of the fractured segments.
Gilmer (1881) described precutaneous osteosynthesis of the jaws by using two posts adjacent to fracture line and lacing their ends together with wire.
Lambotte A (1907) of Belgium reported the fixation of mandibular fractures with a little aluminium plate fixed with two screws.
Roberts WER (1954) postulated that the use of modified thin metacarpal bone plates permitted a stable fixation and eliminated the necessity for intermaxillary fixation.
The earliest mention of osteosynthesis with plates in maxillofacial surgery in England was in 1968, when Luhr HG first published his research on the use of a simplified compression plate and self tapping screws made up of Vitallim for mandibular fracture. He later on worked extensively and developed system of Mini, micro-compression & non – compression plates.
Cook HP (1969) used titanium implants for mandibular reconstruction after the excision of tumours. He found that in addition to exceptional biocompatibility excessive deliberate bending & reverse bending of plates failed to produce metal fatigue or fracture of the component.
Michelet FX et al (1973) introduced the concept of using small, malleable, non- compression vitallium plates and advocated mono – cortical screw fixation in the management of fractured mandible.
Champy M et al (1976) in modification of techniques as used by Michelet et al (1973) described a method of small plates, sufficiently rigid for intermaxilliary fixation to be unnecessary. The plates used were inserted through intraoral route.
Cawood JI (1985) evaluated miniplate osteosynthesis by comparing this technique with intermaxilliary fixation. The plates showed considerable advantage over the other forms of fixation in that they were small, malleable, easy to insert and provide high degree of stability. The rate of recovery of normal jaw function and normal body weight is significantly greater than with intermaxilliary fixation.
Parr GR et al (1985) considered the titanium to be the most biocompatible, corrosion resistant, wear resistant and fracture resistant. Its modulous of elasticity (stiffness) is closer to bone than other implant materials.
Gonzales GA et al(1989) have studied the treatment of mandibular fractures with titanium miniplates. They concluded that the miniplates provide stable fixation as compared to other techniques. The complication rate was very low. They further advocated meticulous technique with passive fittings of the plates.
Schmezeisen R et al (1992) considered 2mm titanium miniplates as a method of choice for treatment of mandibular fractures, as the plates were more rigid and metal released from titanium plates used in mandibular fractures was significantly lower than from stainless steel plates.
Reddy BK & Rajendra K (1995) studied the role of titanium miniplates in delayed osteosynthesis of mandibular fractures. They placed the bone plates through an intraoral approach as described by champy et al, with few modifications. Their study revealed the excellent biocompatibility with high success rate and minimum post – operative complications of titanium miniplates.
Haug RH (1996) considered the titanium and its alloys as permanent implant material in maxillofacial fixation because of its superior corrosion resistance, non- carcinogenicity as compared to stainless steel.
Material & Methods
Subjects for the present study were selected amongst the patients who reported in the department of Oral & Maxillofacial Surgery at Punjab Govt. Dental College & Hospital, Amritsar.
Diagnosis of fracture mandible was made on the basis of detailed history, clinical examination & Radiology examination. Routine laboratory investigations were carried out before undertaking the surgery to evaluate any systemic conditions in these patients.
All the patients were admitted to hospital 24 hours prior to surgery. When the fracture was in dentulous area, the fractured segments were reduced manually & wiring was done on the upper & lower teeth by Erich’s arch bar splints or Eyelet loop method or Risdon’s method of wiring in all the cases for intraoperative maxillomandibular fixation. Operation was carried out under local anaesthesia after proper premedication.
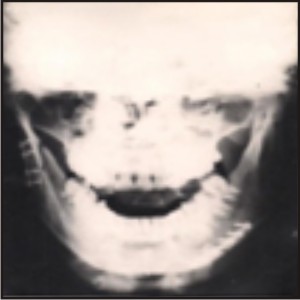 | Case I : Immediate Post Operative
 |
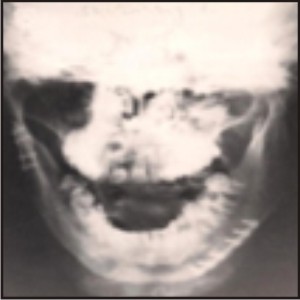 | X-Ray After 5 Months
 |
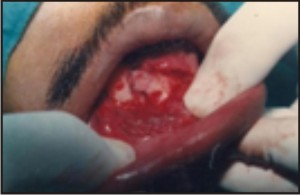 | Case II : Fracture Site Exposed
 |
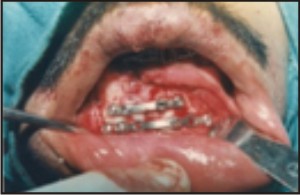 | Mini Bone Plates Fixed
 |
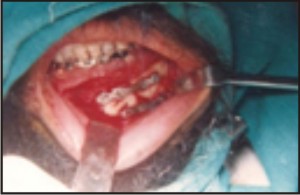 | Case III : Miniplates Fixed At Fracture Site
 |
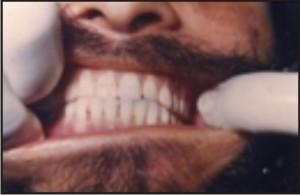 | Post Operative Occlusion
 |
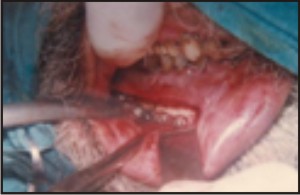 | Case IV : Bone Plate At Fracture Site
 |
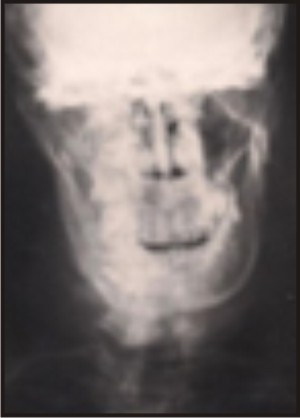 | Post Operative X-Ray
 |
Surgical Armamentarium:
In addition to the armamentarium used for open reduction of mandibular fractures the following instruments were used.
1. Pointed bone reduction forceps.
2. Plate bending pliers.
3. Hand drill (Jacob type)
4. Drill Bits (1.5mm dia.)
5. Screw holding forceps.
6. Self holding screw driver.
7. Universal screw driver.
8. Titanium mini bone plates (4 hole and 6 hole with gap) Dimensions: thickness – 1mm, screw hole dia -2mm.
9. Titanium self tapping monocortical screws.
Dimensions:
Head diameter 4mm,
thread diameter 2mm,
core diameter 1.5 mm,
length of screws 6mm and 8mm.
Operative Techniques:
Under strict aseptic protocol site of operation was scrubbed with Betadine solution. The patient was draped. Local Anaesthesia was administered. The fractured fragments were approached through an intraoral approach or extraoral incision depending upon site of fracture.
Observations
All the patients were males in the age group between 23 – 60 years (mean age 41.5 years)
Road traffic accidents were responsible for majority of the fractures i.e. seven out of ten subjects (70%). In two patients fractures occurred due to fall on the ground (20%). One subject encountered fracture when he was playing football (10%).
Out of eleven fractures, the angle was the most common site (45.4%), followed by parasymphisis (27.3%), body of the mandible (18.2%) and ramus (9,1%). Majority of the fractures occurred on the right side of the mandible (7:4).
Ten patients had eleven mandibular fractures which were treated with fourteen titanium mini plates. Six patients were treated by intraoral approach. In four patients extraoral approach was used for obtaining access to the fracture site.
Major advantages of intraoral technique are the absence of skin scar, possibility of watching simultaneously the reduction of fragments and restoration of occlusion. Extraoral access was used in cases where there was either massive displacement of fragments or intraoral plating was not feasible. Advantages of extraoral approach were better accessibility to fracture site and easy manipulation of fractured fragments.
Post operative complications were encountered in two cases. In the rest of the cases, the healing was uneventful.
Trismus was not observed in any of the operated cases. In four extraoral reductions none of the cases showed hypertrophied scar after the surgery. Paraesthesis of the lower lip was noticed in one of the patients. It resolved in four weeks time post – operatively.
Not a single plate was needed to be removed. There was no clinically visible pigmentation in the tissues.
All the patients showed that following titanium miniplate osteosynthesis of mandibular fractures, restoration of form, function and asthetics was achieved in satisfactory conditions.
Discussion
During the last decade, rigid internal fixation with titanium miniplates and screws had gained widespread acceptance in the management of mandibular fractures. Titanium and its alloys possess outstanding bioacceptability in human body by virtue of formation of oxide film in minimum time and their corrosion resistance to blood and all other body fluids (Haug RH 1996)
Titanium and its alloys are important in dental implants because of their high degree of bioacceptability, strength and corrosion resistance. The high cost of the titanium is the greatest deterrent to its wider use although the cost had reduced over the past ten years. (Parr GR et al,1985)
The present study was carried out on adult patients between the age group of 23 to 60 years. All the cases were males suggesting that males are more prone to trauma. Rix L et al (1991) also reported a high incidence of fractures of mandible in males (90%) in an analysis of 80 cases of mandibular fractures treated with miniplates osteosynthesis.
No damage caused by traumatisation of the marginal mandibular branch of facial nerve was reported post – operatively in any of the patients. Paraesthesia of lower lip was noted in one of the cases. This was probably due to stretching of the mental nerve during retraction. The numbness disappeared in four weeks time postoperatively. Similar observations have been reported by Cawood JI (1985) who cautioned against iatrogenic damage of nerve in management of fracture in the vicinity of mental foramen.
Post – operative malocclusion is reported in patients treated by internal fixation. Inadequate reduction of the fracture, inaccurate maintenance of intraoperative occlusion during plating are stated to be the causes of post – operative malocclusion. In this study postoperative malocclusion was observed in only one patient. Deviation from the original occlusion was treated by retention of elastics for one week and selective grinding. In selected cases intermaxillary fixation for similar reason for a period of seven days post operatively has been recommended by Schmezeisen R et al (1992) where miniplates were used.
The patients were immediately switched to soft oral diet. Patients felt comfortable as intermaxillary was not done and there was early return to work. These findings are in close accordance with results published by Cawood JI (1995); Champy et al (1978); Michelet et al (1973). All the patients showed full range of mandibular movements, did nutritionally well and did not complain of any physical weakness.
Thus as a result of clinical experience, it can be inferred that titanium miniplate osteosynthesis using indigenous titanium bone plates and screw system gives excellent results.
Summary & Conclusions
All the patients were males in the age group between 23 – 60 years. Road traffic accidents accounted for majority of the fractures (70%) followed by fall (20%) and sports (10%). The angle was the most commonly involved site (45.4%) followed by parasymphisis (27.3%), body of the mandible (18.2%) and Ramus (9.1%).
All cases were operated under local anaesthesia through intraoral or extraoral approach using 2.0mm monocortical titanium miniplates and 6mm or 8mm long self threading titanium screws of 2 mm diameter.
Titanium miniplates are malleable, small and easily adaptable to the bone. There was no problem encountered during adaptation of the bone plates. The plates have shown excellent biocompatibility and there was no clinically visible pigmentation. The stability of bone fragments was excellent.
Maxillomandibular fixation was not used postoperatively, but in one patient intermaxillary elastics were kept for one week as slight disturbance in occlusion was noticed. One patient developed infection which resolved with antibiotics and local irrigation with 5% Betadine solution.
It has been observed during the course of this study that titanium miniplates osteosynthesis reduces the period of hospitalisation, patient can early return to work and regular diet. Further there is practically no need for removal of plates and hence second operation thereby bringing down the recurrent expenditure.
Thus it can be concluded that titanium miniplate and screw system exhibits good strength, negligible complications, excellent biocompatibility and good results in the management of mandibular fractures.
Bibliography
1. Bauden JB: Quoted from Krugen E, Schilli W. Oral & Maxillofacial Traumatology, Vol 1,Quintessence publishing Co. Chicago, Page 28, 1982.
2. Brown JS : TrotterM; Cliffe J; Ward – Booth RP; William ED: The fate of miniplates in facial trauma & Orthognathic surgery: A retrospective study. Br. J. Oral & Max. Fac. Surg. 27 :306 – 315, 1989.
3. Cawood JI: Small plate osteosynthesis of mandibular fractures.Br. J. Oral & Max. Fac. Surg. 23, 77,1985.
4. Champy M; Lodde JP; Schimtt R; Mandibular Osteosynthesis by miniplate screws & plate via buccal approach. J. Maxillofac. Surg. 6, 14, 1976.
5. Cook HP: Titanium in mandibular replacement. Br. J. Oral. Surg. 7 : 108 – 111, 1969.
6. Gilmer TL: Citation quoted from kruger E, schilli W. Oral & Maxillofacial Traumatology, Vol 1. Quintessence Publishing Co,Chicago, page 39, 1982.
7. Gonzales GA ; Bermudo AL; Valiente AA; Mateo GJ; Yanez VI: Miniplates in the treatment of mandibular fractures. Rev – Eur – Odontoestomal.1989 Mar – Apr 1 (2): 117 -22.
8. Haug RH: Retention of asymptomatic bone plates used for orthognathic surgery & facial fractures. J. Oral Maxillofac. Surg. 54 : 611 -617, 1996.
9. Lambotte A: Quoted from the article “Removal of asymptomatic bone plates used for orthognathic surgery & facial fractures”. J. Oral Maxillofac. Surg. 54 : 618 -621, 1996.
10. Luhr HG : Compression plate osteosynthesis through the Luhr system. Quoted from kruger E. Schilli W. Oral & Maxillofacial traumatology, Vol 1. Quintessence Publishing Co. Chicago, page 349, 1982.
11. Michelet FX; Deymes J ; Dessus B : Osteosynthesis with miniaturized screwed plates in Maxillo- facial Surgery.J. Max. Fac. Surg. 1 :79 :84, 1973.
12. Miller BG; Frame JW; Browne RM : A histological study of stainless steel & titanium screws in bone. Br. J. Oral& Max. Fac. Surg. 28 :92-95, 1990.
13. Parr GR; Gardner LK; Toth Rw: Titanium : The mystery metal of implant dentistry. Dental material aspects. The journal of Prosthetic Dentistry 54 : 410 – 414, 1985.
14. Reddy BK ; Rajendra K: Delayed osteosynthesis of mandibular fractures with titanium miniplates. Ind. J. Oral & Maxillofac. Surg. X1, 11 – 20, 1995.
15. Rix L ; Stevenson RL ; Punni – MoorthyA: An Analysis of 80 cases of mandibular fractures treated with miniplate osteosynthesis. Int. J. Oral & Max. Fac. Surg. 20 :337 – 341, 1991.
16. Robert WR : The cases of mandibular plating. Br. J. Oral max. Fac. Surg. 1 :200, 1964.
17. Schmelzeisen R; Mc Iff T; Rahn B: Further development of titanium miniplate fixation for mandibular fractures. Experience gained & questions raised from s prospective clinical pilot study with 2.0 mm fixation plates. J. Cranio Max. Fac. Surg. 20 :251 – 256, 1992.
18. Wald RM Jr ; Abemayor E ; Zemplenyi J ; Mannai C ; Lesavoy MA: The transoral treatment of mandibular fractures using non – compression manipulates: A Prospective Study. |